Diabetic foot ulcers: understanding, preventing, and managing the risks
Written by the editorial staff writer at Hola. Medically Reviewed by Dr Nelson Lau, MBBS FRACGP, GP & Digital Health Specialist. Dr. Ammar AL-ANI, MBChB, CCBST, AMC. Blog updated on 25 November, 2025. Originally published on 19 November, 2024.
Contents

Overview
Foot ulcers are among the most common but preventable problems for people with diabetes in Australia. A diabetic foot ulcer is an open wound or sore on the foot or lower leg that heals slowly as high blood sugar damages nerves and reduces circulation. Awareness and early care are vital because, without prompt attention, such ulcers can result in serious infection or even amputation (limb loss). Recent Australian data1 suggest that roughly 15% of people with diabetes may experience a foot ulcer at some point.
Medical Disclaimer: The information in this article is for educational and research purposes only and does not constitute professional medical advice, diagnosis, or treatment. In an emergency, call 000 immediately.
What is a diabetic foot ulcer?
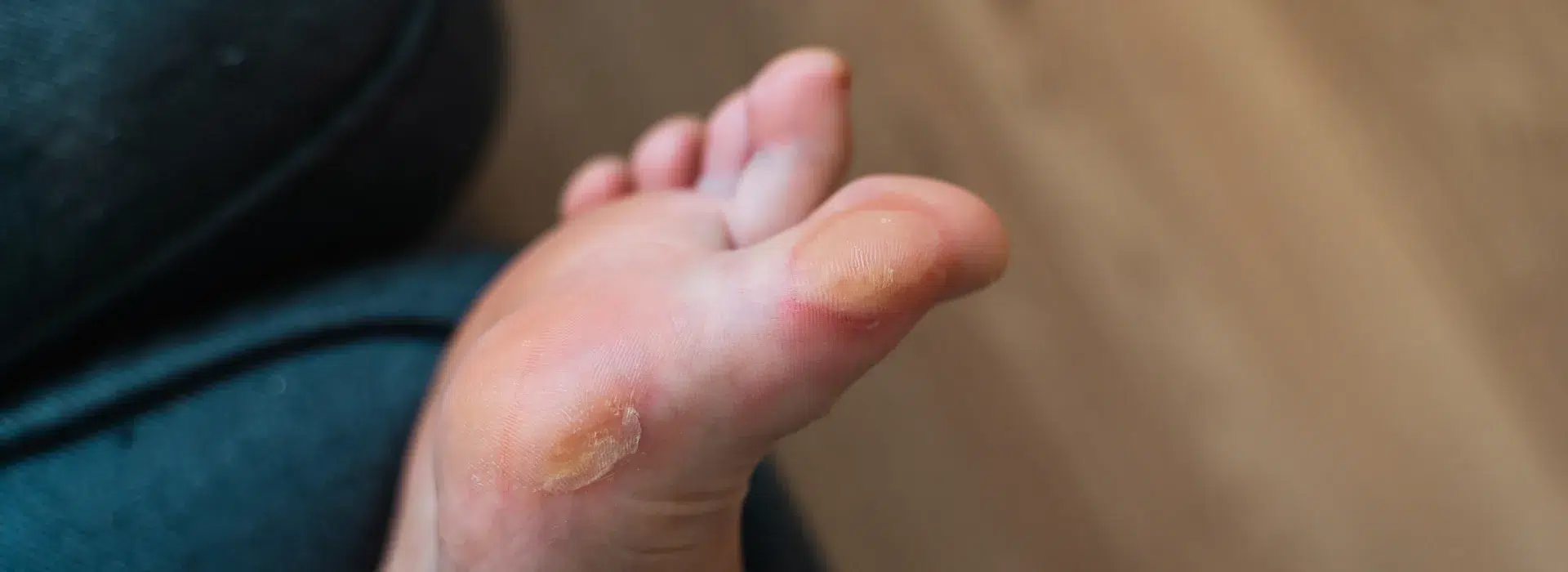
A diabetic foot ulcer is a slow-healing wound on the foot or lower leg. Elevated blood sugar levels over time can damage nerves and blood vessels, making it difficult to notice cuts, blisters, or pressure points. Additionally, impaired circulation can slow down the healing process. Ulcers often develop in areas exposed to pressure or friction, such as under the big toe, heel, or the ball of the foot.
Causes
Common contributing factors include:
- Poor blood circulation (such as from peripheral arterial disease) limits oxygen and nutrients from reaching the skin and tissues.
- Nerve damage (neuropathy) may lead to loss of feeling in the feet. As a result, small cuts or tight footwear can go unnoticed.
- High blood sugar levels slow the healing process, increasing the risk of infection.
- Foot injuries or pressure points, such as from tight shoes, standing for long periods, cuts, or blisters, can trigger ulcers if not detected early.
- Infections can easily develop and worsen due to sensory loss.
- Smoking further reduces blood flow and impairs healing.
Symptoms & warning signs
If you have diabetes, check your feet every day (especially if you have nerve damage). Watch out for:
- Persistent sores or wounds that don’t heal
- Redness, swelling, or warmth around a wound
- Drainage or an unpleasant odour from an open sore
- Calluses or blisters that break open
- Numbness, tingling, or burning sensations in your feet
If you notice any of these, act early—early action can prevent serious complications.
Complications if left untreated
If a foot ulcer is left untreated or not properly managed, the risks may become serious. Possible complications include:
- Infection can spread into the skin, underlying soft tissue, bone, or bloodstream.
- Gangrene (tissue death) may develop if the blood supply is poor.
- Amputation risk—in severe cases, infection or gangrene may lead to part of the foot or leg being removed. In Australia, more than 4,400 diabetes-related amputations occur each year.2
- Reduced mobility, poor quality of life, and longer hospital stays.
Note: Most ulcers are preventable with prompt action and early care.
Feeling unwell? Consult an Australian-registered GP online, 24/7.
Prevention tips
Here are some practical, clinically recommended prevention tips you can follow:
- Check your feet daily: Look for cuts, blisters, redness, or swelling.
- Keep feet clean and dry: Wash gently, especially between toes, and dry thoroughly.
- Moisturise regularly: Use a moisturiser to keep your skin soft and crack-free, but avoid applying between toes.
- Wear proper footwear: Choose comfortable, well-fitting shoes that allow room for movement and guard against friction and injury.
- Trim toenails carefully: Trim your toenails straight across to prevent ingrown nails.
- Don’t walk barefoot: Always wear footwear, even at home. Small household injuries can easily turn into ulcers.
- Control blood sugar: Keep glucose levels within the target range to protect your nerves and circulation.
- Stop smoking: Quit smoking, as it improves circulation.
- Schedule regular foot checks with your GP or podiatrist: Have regular foot assessments with your GP, especially if you have neuropathy or poor blood flow.
Managing an existing foot ulcer
If a foot ulcer develops, here’s what you should do:
- See a doctor immediately for assessment.
- Keep the wound clean and covered with sterile dressings.
- Follow medical advice on meds or special footwear.
- Avoid pressure on the affected foot (use crutches or special shoes if advised).
- Monitor healing progress — even small ulcers can worsen quickly in people with diabetes.
When to see a doctor
You should contact a healthcare provider (GP or podiatrist) or book an online consultation if any of the following occur:
- A foot sore doesn’t heal within a week
- There’s swelling, redness, pain, discharge, or unpleasant odour from a wound
- You can’t feel your feet properly (numbness)
- You have a history of foot ulcers or poor circulation
- One foot feels significantly hotter or colder than the other.
Note: Early action is key to preventing escalation.
How Hola Health can help
At Hola Health, our Australian-registered doctors can provide initial medical advice and help you evaluate your conditions. Online GPs can provide referrals to specialists and assist with management if clinically indicated.
- Risk Assessment: Our GPs can help identify if your symptoms require urgent hospital care or a specialist referral.
- Pathology & Referrals: We provide pathology referrals if appropriate.
- Education: Our telehealth doctors provide advice on footwear and self-care to prevent ulcers from forming.
Clinical note: A diabetic foot ulcer is a medical priority that requires an in-person physical assessment, including vascular and neurological testing. Telehealth cannot replace a physical examination for an active wound. Ulcers require a team (Podiatrist, GP, and often a Vascular Surgeon), not just a standalone online GP, typically. If you notice a new ulcer, swelling with fever, or your foot turns black/blue, call 000 or visit an Emergency Department immediately.
Conclusion
Diabetic foot ulcers are a serious yet largely preventable complication of diabetes. With daily care, vigilance, and timely medical support, most cases can be avoided. For Australians living with diabetes, staying proactive about foot care and seeking help early can support long-term well-being. Don’t wait for symptoms to worsen; connect with a healthcare professional as soon as you spot anything unusual.
FAQs
What causes diabetic foot ulcers to form?
They develop when high blood sugar over time causes nerve damage (neuropathy) and impairs circulation, leaving the feet more prone to injury and delayed healing.
Can I treat a diabetic foot ulcer at home?
Diabetic foot ulcers should not be self-treated. While you play a vital role in daily care, professional medical oversight is mandatory to prevent infection and monitor healing progress.
How long does it take for a diabetic foot ulcer to heal?
Healing time varies depending on the ulcer’s size, depth, infection, blood supply, pressure management, and blood sugar control. Recovery may take weeks to months, and some individuals may experience persistent symptoms for months or longer.
Are foot ulcers preventable if I manage my blood sugar well?
Yes, managing blood sugar well can significantly reduce the risk of nerve and circulation damage that can lead to ulcers. With consistent foot care and check-ups, prevention is highly achievable.
Can I get diabetic foot care online in Australia?
Yes, many services (including Hola Health) offer online GP consultations, referrals, prescriptions, and guidance. However, an in-person physical assessment is required for any active ulcer to evaluate circulation, nerve damage, and wound depth.
Need to see a specialist? Request your specialist referral with Hola Health.
Reference
- Prevention, identification, and management of foot complications in diabetes - reference link
- Diabetes Australia - reference link
Providing consult for
- Cough
- Nausea & vomiting
- Fever
- Hayfever
- Fatigue
- Sore throat
- Acne
- Gout
- Eczema
- Rosacea
- Sunburn
- UTI
- Erectile dysfunction
- Contraception
- Morning sickness
- Morning after pill
- Prostate health
- Anxiety
- Depression
- Stress
- Grief & loss
- Premature ejaculation
- Asthma
- Blood pressure
- Diabetes
- Cholesterol
- Migraines & headaches
- Allergies
- Heartburn & reflux
- Sleep disorder
- Gastro
Related Articles
Disclaimer
This blog is for general informational purposes only and does not indicate that Hola Health provides all treatments or preventive measures mentioned. It is not intended to be a substitute for professional medical advice. Always seek the guidance of your doctor or other qualified health professional with any questions you may have regarding your health or a medical condition. For emergencies please immediately contact 000. Any medical topics discussed are intended to educate, not to imply availability through Hola Health.




